
So lovely to get this feedback from my gorgeous client about mine and Julie’s @eternalwellbeingcanberra first podcast!
#BeyondTheMirrorRedefiningBeautyAndWellness#podcast#AustralianPodcast#BeautyPodcast#WellnessPodcast
I’d love your feedback on the podcast so far. If you have any comments, or questions – hit me up and we can tackle it in a future podcast!
Here’s a link to click through and have a listen: https://open.spotify.com/show/6h6wN1ku87PKUhL3p4yaTC
Peninsula Endermologie Clients will already know that they’re getting expertise in the “Top 10 Trends” predicted for 2025. Imagine nailing all but one of these trends (soz, no botox here), in just one, truly non-invasive treatment!!! Pretty good hey? Click on the image below to read the full article.
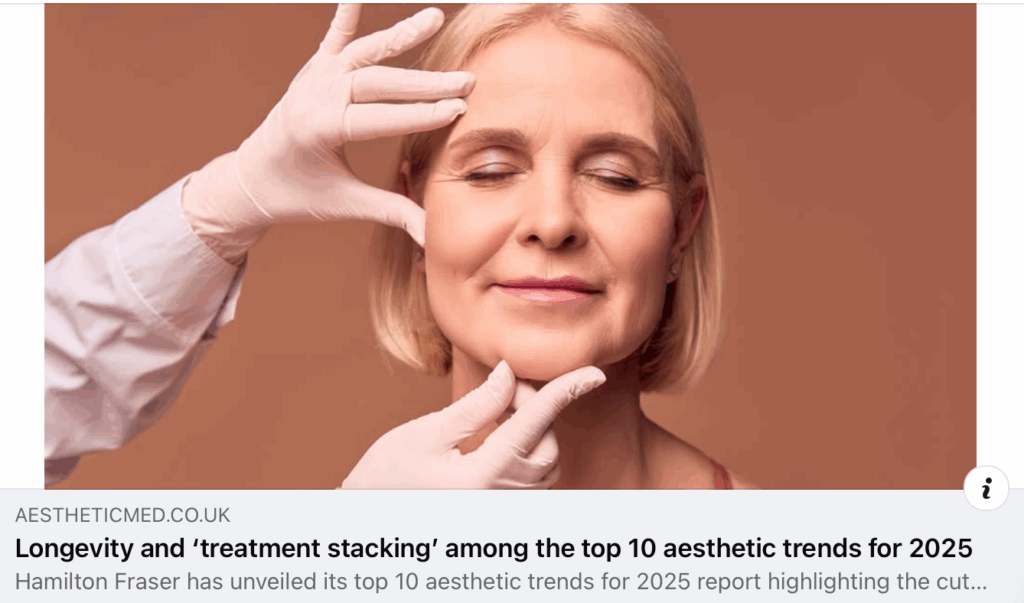
If you don’t have time to read the article, in a nutshell the trends are:
1. Longevity/ biohacking – individualised treatments that support the pillars of healthy ageing, such as nutrition, movement, sleep, stress management, cognitive activity & social/spiritual connection. Endermologie ![]()
2. Regenerative aesthetics – natural, long-term rejuvenation by stimulating the body’s natural healing processes & helping bank valuable collagen. Endermologie ![]()
3. ‘Less is more’ – The end of overfilled faces. (Hurrah)! Endermologie ![]()
4. Treatment ‘stacking’ – combining treatments, i.e. using multiple modalities at the same time, is the latest term de jour. Endermologie ![]()
5. Personalisation – bespoke treatments. Endermologie ![]()
6. Weight loss meds – and supporting the skin as you lose weight rapidly. Endermologie ![]()
7. Regulation – Increased regulation & legitimisation of aesthetic procedures as medical treatments. Again, HURRAH!! Endermologie ![]()
8. Advances in botulinum toxin/botox – longer-lasting formulations & improved injection techniques.
9. Hair loss treatments – Hair and scalp health. Although there’s no clinical evidence for Endermologie with hair growth yet, it does stimulate blood and lymphatic circulation, so could help in theory ![]()
10. Women’s health and menopause – increased demand for holistic care. You know I got you ladies!!! Endermologie ![]()
- Introduction of Medicare-funded Menopause Health Checks: The Australian government is introducing a Medicare rebate for menopause health assessments. These comprehensive evaluations, typically lasting 45 minutes to an hour, will assess various aspects of a woman’s health and wellbeing during menopause. The Australian
- Significant Investment in Women’s Health: A commitment of over $500 million has been pledged to enhance women’s health services over the next five years. This includes improved training for medical professionals, expanded access to subsidized menopausal hormone therapies (MHT), and the establishment of specialist menopause clinics. The Australian+1The Australian+1
- Expansion of Specialist Menopause Clinics: New multidisciplinary menopause hubs are being established, such as the one in Randwick, NSW. These clinics cater to women experiencing severe or complex menopause symptoms, providing individualized treatment plans developed by a team of specialists. The Australian
- Inclusion of Mental Health Support: Recognizing the psychological impact of menopause, these clinics also offer mood clinics to address mental health concerns, an area previously neglected in menopause care. The Australian
- Broader Access to Subsidized Therapies: The Pharmaceutical Benefits Scheme (PBS) will now include additional MHT options, aiming to make these therapies more affordable and accessible to women in need. The Australian+1The Australian+1
- Addressing Cardiovascular Risks: The initiative also emphasizes the importance of monitoring heart health during menopause, as declining estrogen levels can increase the risk of cardiovascular diseases. dailytelegraph
- Political Bipartisanship: Both major political parties in Australia have shown support for these initiatives, indicating a shared commitment to improving women’s health services nationwide. The Australian
These developments represent a significant step forward in acknowledging and addressing the health needs of women undergoing menopause in Australia.
Did you know your brain has a lymphatic system (aka waste-disposal system) of its very own? It’s called the glymphatic system and it activates at night while we sleep (the opposite of the lymphatic system that’s more active in the day).
I’m just mentioning it now because I’ve had this conversation twice this week explaining the importance of sleep – always – but particularly in peri-menopausal women who suffer from insomnia. Getting a good night’s sleep is essential for our long-term brain health, so we really need to make it a priority. I can share some tips on how to do just that in the next few days. Here’s an interesting study that looks at the effect of sleep on glymphatic drainage:

For the data nerds, it’s worth taking a look at the study – but here’s essentially what it says…when we fall asleep, our brain stops paying as much attention to the outside world and switches to ‘maintenance’ mode. During sleep, the waste from the brain is ‘flushed’ out using a system called the glymphatic system. However, until recently, scientists weren’t sure exactly what controls this cleaning process.
In this study, researchers used advanced technology to track different signals in the brain during non-REM (NREM) sleep. They found that norepinephrine (a brain chemical related to alertness), blood flow in the brain, and cerebrospinal fluid (CSF) movement were all key for waste removal.
When they used light to stimulate a specific brain region called the locus coeruleus (which affects norepinephrine levels), it changed the way blood vessels pulsed and how CSF flowed in the brain. They also found that making blood vessels pulse more strongly helped CSF flow into the brain, acting like a pump to push waste-clearing fluid through.
On the other hand, when they gave the common sleep medication “zolpidem”, it reduced norepinephrine fluctuations and slowed down the brain’s cleaning system. This suggests that norepinephrine and blood vessel movement are essential for clearing out waste during sleep.
In short: the brain’s waste-clearing system (glymphatic) works best when norepinephrine levels rise and fall in sync with blood flow and CSF movement during DEEP sleep. Medications that interfere with this rhythm may slow down this cleaning process.
Following on from my last post, I want to briefly expand on why sleep isn’t just about rest.
During sleep, your brain cleans out waste that builds up throughout the day, including harmful substances like β-amyloid that have been linked to diseases like Alzheimer’s.
This is called the glymphatic system. Since some things can’t pass through the brain’s protective barrier, this system uses fluid to move medicine in and flush toxins out. It also helps bring nutrients, such as glucose, lipids, amino acids, growth factors and neuromodulators, into the brain to keep it healthy..
So skimping on sleep doesn’t just make you tired – it affects everything from your immune system to mental health. Poor sleep can directly cause:
– Higher risk of anxiety, depression, and brain fog
– Increased likelihood of weight gain and cravings
– Reduced immune function
– Worsened skin health and premature ageing
Stay tuned for some tips on improving your sleep!

OK, so we’ve established that sleep is necessary for good health. Let’s explore some simple sleep hacks for a better night’s rest ![]()
![]()
Better sleep starts with good habits.
Set a consistent bedtime, aiming to get at least 8 hours a night. More if you can. Your body loves routine, so aim for the same time every night.
Keep your room cool, dark & quiet – Ideal temp: 16–19°C. This is said to emulate the cave-like conditions humans adapted to!
Avoid caffeine in the afternoon/evening. This is individual. I know some people who seem to tolerate caffeine much better, but it’s best to avoid it in the afternoon if sleep is a problem.
No screens before bed – blue light blocks melatonin – the hormone we need to get a long, restful night sleep.
Try relaxation techniques – reading (though probably not true crime), stretching, or breathing exercises to help you wind down (and lower cortisol) before bedtime.
Limit alcohol and heavy meals late at night – the energy required to digest the food and detox from booze will disrupt deep sleep.
Endermologie is proven to reduce stress and improve sleep. Book in for the VSS protocol (vitality, stress & sleep).
Which of these do you already do? Any tips that work for you?

Here’s the last of these posts relating to sleep (for a while). While it’s clear that getting a good night’s sleep is essential for good health, it’s not always so easy for some people. If you’re struggling it’s a good idea to start with the suggestions in my last post.
But remember that a good sleep routine starts before you get into bed. You might need to look at why your cortisol (aka stress) levels are elevated during the day and implement some changes to reduce stress (e.g. exercise in the morning, deep breathing regularly throughout the day, meditation, grounding with a swim or walk outside etc.)
I also love magnesium supplements to help with my restless legs and improve sleep. (A bath with epsom salts will help too). Some people swear by valerian root and/or chamomile. Melatonin is OK for short-term use – e.g. to help regulate your sleep cycle after jet lag. And there are always prescription drugs if your insomnia is becoming chronic or you’re going through a particularly stressful time.
If you’re still not having much luck, here are a few more ideas to help you create a nighttime wind-down routine:
30 mins before bed: Dim the lights, put away all screens
20 mins before bed: Light stretching, reading, or journaling
10 mins before bed: Deep breathing or meditation
Lights out!
Try this for a week and let me know if it helps!
If you want to nerd out for 5 mins on the reasons I added Sea Buckthorn to my Anti-Cellulite Body Oil. Click on the image below to read the Medscape review:

Read the rest of the Anti-Cellulite Body Oil ingredients here.
Product Details
This lush anti-cellulite body oil leaves the skin feeling noticeably more smooth, supple & firmer.
An exquisite blend of essential oils pampers the senses & stimulates the skin’s natural powers of self-regeneration. Rosemary, grapefruit, lemon, cyprus, carrot, seabuckthorn & fennel-sweet increases circulation, relieves fluid retention & flushes away toxins, while cinnamon bark & witch hazel refines & tightens your skin.
Blended with anti-oxidant and vitamin-rich grapeseed & avocado oils for perfect absorbtion.
How to use: Use twice a day after your shower. Best applied whilst the skin is still damp, or after a gentle towel-dry. Shake the bottle before you pump and remember, a little goes a long way! Spend as much time as you can massaging this nourishing oil into your skin. Your body will thank you for it!
Hint: Dry body brush before your shower to exfoliate away your dead skin cells, boost your circulation and allow a better application and penetration of the body oils into your skin.
All natural, all organic and toxin free.
Made with love at Peninsula Endermologie HQ.
So good to see more cosmetic surgery doctors recommending LPG Endermologie. It’s brilliant Pre and Post Op.



Thanks to @lpgendermologie_uk for sharing!
![]() FEATURE ALERT!
FEATURE ALERT! ![]()
We’re beyond proud to see LPG![]() featured in Tatler’s Beauty & Cosmetic Surgery Guide 2025 as a key treatment recommended by two of the UK’s Top 50 Doctors!
featured in Tatler’s Beauty & Cosmetic Surgery Guide 2025 as a key treatment recommended by two of the UK’s Top 50 Doctors! ![]()
A huge congratulations to @atelier.dr.aggie and @drsabrinashahdesaiofficial on this incredible recognition! ![]()
![]() Your dedication to aesthetic excellence and skin health is truly inspiring, and we’re honoured to be part of the cutting-edge treatments you trust.
Your dedication to aesthetic excellence and skin health is truly inspiring, and we’re honoured to be part of the cutting-edge treatments you trust.
A special thank you to @francescaogiermannwhite and the team at @tatlermagazine for this fantastic edition, highlighting the very best in aesthetic innovation.
Here’s to advancing beauty through Cellular rejuvenation, skin regeneration, and the power of LPG![]() !
! ![]()
#ProudPartner #2025 #aesthetics

Love that @endotherapeutics.aesthetics and @scarlesstheclinic are spreading awareness of LPG Endermologie treatments to Doctors across Australia. See that gorgeous Alliance machine peeking in the right hand side of the image? It’s the same as the one right here in Mt Eliza.
Posted @withregram • @scarlesstheclinic Scarless is proud that our Director Dr Andrea Issler-Fisher had the honor of chairing the multidisciplinary conference hosted by ESPH today at the Hilton Sydney.
The event showcased outstanding, high-quality presentations from some of Sydney’s most esteemed surgeons across various specialties.
With 150 GPs in attendance, it was a fantastic opportunity for collaboration and knowledge sharing. We extend our gratitude to ESPH for organizing this exceptional event, our gold sponsor Endotherapeutics for their invaluable support, and to all the delegates for their participation.
We are proud of our Director’s continued commitment to advancing surgical practices and representing Scarless at such prestigious gatherings!

Thanks to Mark Sisson for explaining this rationally so I don’t have to…
What’s up with the alkaline diet?
When we metabolise foods, we produce metabolic waste products of various pH levels. Foods like meat, fish, grains, legumes, and dairy generate what’s called an acidic ash, and they’re often lumped together under the label of “acid-forming foods.” Many proponents of the alkaline diet argue that regularly eating these foods causes the body to become chronically acidic, leading to bone loss, poor performance, and degenerative disease.
But here’s what’s actually true.
Your Body Regulates Blood pH on Its Own
The body has multiple overlapping systems for regulating pH. First, there’s respiration. The lungs maintain blood pH by modulating how much carbon dioxide (CO₂) we exhale. This is instantaneous and incredibly precise.
Then there are the kidneys. They excrete hydrogen ions when the body’s too acidic and regenerate bicarbonate ions to buffer the blood. This takes a little longer, but it’s highly effective.
As long as your lungs and kidneys are functioning properly, the pH of your blood doesn’t budge. It doesn’t matter what you eat. Yes, eating more meat can make your urine more acidic, but that’s proof your kidneys are doing their job and offloading the excess acid.
Chronic acidosis, the kind that alkaline diet proponents are talking about, only happens when these systems fail. These failures don’t happen because of “increased acidity” from grass-fed steaks and yogurt. Instead, they’re caused by untreated diabetes, alcohol abuse, and other serious maladies.
Acidic Diets and Bone Health
The other big claim is that acid-forming diets leach calcium from the bones in an attempt to buffer the acidic load. This sounds plausible at first. Studies show that urine calcium increases after eating protein. Peeing out calcium sounds bad, right?
Yes, eating protein increases urinary calcium, but it also increases calcium absorption in the gut. The net effect is neutral, or even positive, for bone health. You’re not peeing out bone calcium. You’re urinating out the excess calcium that the protein helped you absorb.
We know this because real-world studies consistently show that higher animal protein intake improves bone mineral density and reduces fracture risk, especially when paired with adequate calcium. It helps that most of the protein-rich foods we recommend, like meat, eggs, dairy, and gelatinous bone broth, also come bundled with the very nutrients you need to metabolise and buffer any acid they generate.
What About People With Compromised Kidneys?
Here’s where the concern might be warranted. People with kidney disease or declining renal function do have a reduced ability to excrete acid. That can lead to low-level acidosis and real consequences.
However, in people with healthy kidneys, adding “extra” animal protein actually improves kidney function and makes it even easier to buffer acidity by providing ammonia substrates. The alkaline diet people would predict the opposite, and they would be entirely wrong.
A Rant About Biohacking pH
The alkaline diet crowd ultimately believes they can improve upon millions of years of human evolution and physiological development by top-down micromanaging your acid-base balance.
Like every other group that tries to wrest control of an incredibly intricate system, this will end badly. You don’t outsmart your kidneys. You support them with a nutrient-dense diet and trust them to do their job.
Sodium Bicarbonate for Performance
There is one valid use case for “alkalising” your body: intense training. One of the most consistent findings in sports nutrition is that taking sodium bicarbonate (baking soda) before a workout improves performance, power output, and endurance. It buffers the acute acidity that builds up during intense exercise, delaying fatigue.
The sweet spot seems to be between 0.2 and 0.4 grams per kilogram of bodyweight. Too much can cause bloating, nausea, and full-blown GI distress.
Final Thoughts
You can’t alter your long-term blood pH through diet. If you could, you’d be in the ER. If the alkaline diet helps someone eat more whole foods and vegetables, that’s a win. But it’s not because they’re “neutralizing acid” in their bloodstream—and since they’re also omitting meat, seafood, dairy, and eggs, they’re actually worsening their nutrient intake.
If you’re worried about acidity dissolving your bones, focus on mineral intake—magnesium, potassium, calcium, and sodium—and getting enough quality dairy and animal protein. Don’t avoid steak because someone on Instagram told you it turns your bones into chalk.
It’s total nonsense, and the opposite is true.
Julie @eternalwellbeingcanberra and I had the privilege of chatting with the incredible Maria Veracruz on ‘Beyond the Mirror’ podcast!
Maria is a physiotherapist, internationally renowned medical Endermologie expert and trainer, with over 21 years of experience in the field.
Maria describes Endermologie as “not just a treatment, it’s a real transformation”. It’s a journey to discover your body’s potential.
Endermologie is a non-invasive, very safe approach used for rejuvenating, restoring, and revitalising the body. It’s been around for nearly 40 years and is established across the world.
Maria champions a natural approach and helps clients understand and embrace their bodies, including their fat cells, which serve essential functions. This holistic treatment supports both aesthetic goals and overall health. Clients often report feeling lighter, refreshed, rejuvenated, and experiencing better sleep and increased energy after treatments. This can lead to a “lifestyle affirmation” and motivates people to make positive changes like exercising and eating better.
This conversation highlights the importance of body acceptance, embracing natural aging, and making conscious choices for your well-being.
This podcast helps get the word out that Endermologie is a natural, versatile option that can treat many conditions and support overall wellness.
Let me know what you think once you’ve tuned in!
#Endermologie #WellnessJourney#BodyTransformation #FacialRejuvenation#PainManagement #HolisticHealth #SelfCare#NonInvasive #BeautyExpert #Vitality#BodyConfidence #HealthAndWellness
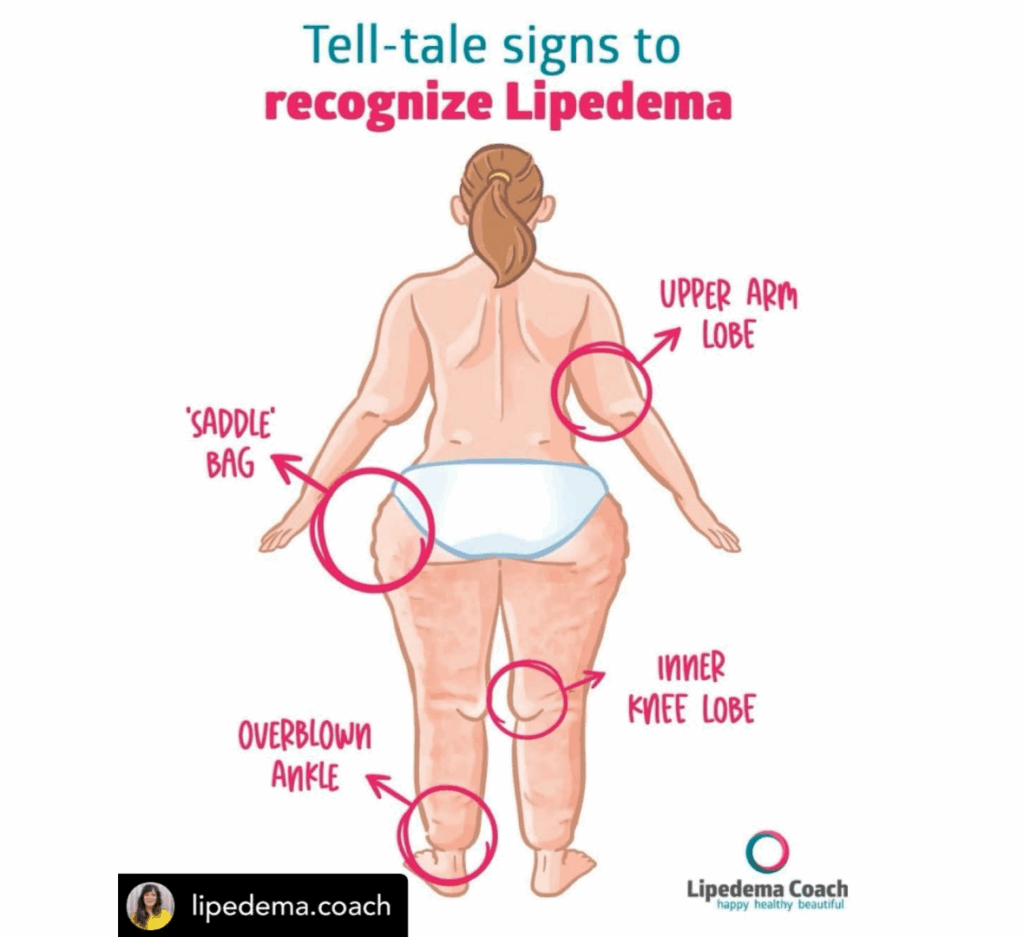
Reposted with thanks to @lipedema.coach
Is Lipedema still misdiagnosed in 2025? Sadly, Yes ![]()
Even today, women with Lipedema continue to go undiagnosed for years, even decades. And week after week in my practice, I hear the same story:
![]() A woman starts noticing something’s “off” as a teenager. Her legs feel heavy, painful, and never seem to respond to diets or exercise the way the rest of her body does.
A woman starts noticing something’s “off” as a teenager. Her legs feel heavy, painful, and never seem to respond to diets or exercise the way the rest of her body does.
![]() She goes to her doctor, maybe even a few.
She goes to her doctor, maybe even a few.
![]() She’s told it’s just weight gain. Hormones. Salt. Genetics.
She’s told it’s just weight gain. Hormones. Salt. Genetics.
![]() She tries everything—restrictive diets, workouts, compression stockings—and still, nothing changes.
She tries everything—restrictive diets, workouts, compression stockings—and still, nothing changes.
It often isn’t until her thirties or beyond that she finally hears the word Lipedema for the first time. And by then, the symptoms have progressed, the pain has increased, and the emotional toll has grown heavy.
This is exactly why I do what I do.
Lipedema is a progressive condition, which means early recognition makes all the difference. And it starts with knowing what to look for!
Some of the most commonly seen Lipedema symptoms:
![]() Noticeable size difference between upper and lower body
Noticeable size difference between upper and lower body
![]() Fat build-up in specific areas (like saddlebags or knee lobes)
Fat build-up in specific areas (like saddlebags or knee lobes)
![]() Pain and tenderness, even without pressure
Pain and tenderness, even without pressure
![]() Easy bruising for no clear reason
Easy bruising for no clear reason
![]() Cold sensations, especially in the legs or buttocks
Cold sensations, especially in the legs or buttocks
![]() Skin that feels lumpy or uneven underneath
Skin that feels lumpy or uneven underneath
![]() Heavy, tired legs, even with minimal activity
Heavy, tired legs, even with minimal activity
Other tell-tale signs include:
![]() No response to diet or exercise
No response to diet or exercise
![]() Swelling or fluid retention
Swelling or fluid retention
![]() Symptoms worsening into secondary lymphedema
Symptoms worsening into secondary lymphedema
![]() Increasing mobility issues or joint pain
Increasing mobility issues or joint pain
If this sounds familiar, you’re not imagining it, and you’re not alone.
![]() Keep asking questions.
Keep asking questions.
![]() Keep learning.
Keep learning.
![]() And keep fighting for the care you deserve.
And keep fighting for the care you deserve.
Let’s make early recognition the norm, not the exception.
With love,
Rachel – Founder at Lipedema Coach
![]() @krijlcreatie
@krijlcreatie
Rant incoming…
Now I know this VERY young lady is just trying to create reels that will please the Google Gods, but isn’t anyone else sick and tired of taking “anti-ageing” advice from a child? This kid looks like she’s barely out of her teens and is lecturing us oldies about how to stay forever young.
First of all – WE’RE ALL GETTING OLDER – YOU CAN’T STOP IT!
Secondly – WE’RE ALL GETTING OLDER. YOU LITERALLY CAN’T STOP IT.
There’s absolutely NOTHING that can stop us from getting older. Sure, you can have a crack at being Bryan Johnson for a few weeks/months/years if you really hate the life you’re living – but guess what – you’ll still get older.
And as for getting older but trying to look younger – “THE SECRET” (as this young lady suggests) – I don’t think there’s a single person alive past 18 who doesn’t know that we SHOULD wear sunblock, drink enough water, exercise and eat good food. Then throw in a few public health measures like vaccination, plumbing, don’t smoke or take recreational drugs and handwashing and you’ve got the “secret” to living as long as possible right there.
And look, I’ve probably been guilty of using the expression myself back in the day, but as I go gratefully towards the latter stage of my life, I’m far more concerned than feeling good and looking healthy than trying to look younger.
So could the Internet please just back off and let us age heath-fully rather than keep trying to tell us we can’t age.
Thank you.
#positiveageing
RePosted with thanks to @getthegloss
Yes please! A salon treatment that zaps your cellulite and your stress at the same time ![]()
LPG Endermologie is the iconic ’90s cellulite massager and it used to be pretty uncomfortable, but beauty editors loved it ![]()
Now it’s had a major upgrade and comes with other proven wellness benefits, reducing cortisol by 19% in a single session, 55% fewer sleepless nights, and possibly even a mild Ozempic-like effect ![]()
So long as you wear the body stocking! GTG’s @theogbeautyboss and @victoriawoodhall try it out ![]()
Scars tell a story – of healing, survival, transformation and strength.
But even well-healed scars can create discomfort, sensitivity, tightness or restricted movement long after the surface looks repaired.
Whether a scar is the result of surgery, trauma, burns, C-section, mastectomy, joint repair or liposuction, the deeper layers of tissue may heal in a way that feels stiff, tethered or uneven.
We call this fibrosis – dense, inflexible bands of collagen that limit glide and mobility between tissue layers.
While scar appearance often receives the most attention, the feel and function of the scar are just as important for comfort and body confidence.
How scars can affect the body
Even a small incision can influence tissue behaviour throughout a much larger region.
Common experiences include:
- Tightness, pulling or restriction with certain movements
- Reduced range of motion
- Tingling, numbness or hypersensitivity
- Local swelling or congestion, leading to a build up of stubborn fat
- Irregular contouring or surface dimpling
- Discomfort, heaviness or protective bracing around the area
This happens when scar tissue forms rapidly and densely during the early stages of healing. Rather than the smooth, organised collagen we want, it can develop in thick bundles that restrict glide between skin, fascia and muscle layers.
Where Endermologie can help
Endermologie supports scar and fibrosis healing by using gentle mechanical stimulation to:
- Improve circulation and oxygen delivery to the tissue for improved healing¹
- Mobilise lymphatic fluid to reduce congestion²
- Encourage collagen remodelling for improved texture and appearance²
- Soften dense or adhered areas to restore glide³
- Improve mobility and range of motion³
- Reduce sensations of tightness, heaviness or pressure³
- Support nerve desensitisation and comfort over time³
This is achieved without heat, cutting, needles or aggression, which makes it ideal for sensitive or complex surgical histories.
Which scars can benefit?
Endermologie was first developed to treat scars, so it can promote healing in the following and more:
- C-section
- Liposuction
- Tummy tuck / abdominoplasty
- Breast augmentation, reduction, lift & explant
- Mastectomy & reconstruction
- Joint replacement
- Orthopaedic repair
- Post-cancer radiation fibrosis
- Burn scarring
- Injury or accident trauma
- Adhesions or fibrosis affecting posture, mobility or appearance
When treatment can begin
Timing is individual and guided by medical clearance.
General guidance suggests:
- Once incisions have closed and wound has closed (typically 2–3 weeks post-op¹)
- Earlier in specialist cases (e.g. lymphatic congestion following node removal – always surgeon-approved)
- Months or years later to address established fibrosis or movement restrictions
It is never too late – scar tissue continues to remodel for years.
What results feel like
Clients commonly report:
- Softer, more flexible tissue
- Reduced tightness or pulling
- Smoother contour and reduced visible puckering
- Improved comfort with movement
- Less sensitivity or numbness
- Feeling more at home and confident in their body
Changes are gradual, cumulative and respectful – not forced.
Why training and anatomical expertise matter
Endermologie is exceptionally safe when delivered appropriately, but scar and fibrosis work requires clinical understanding.
Niamh is a former Registered General Nurse with extensive experience caring for patients pre- and post-operatively within cosmetic and reconstructive surgery, and is a Certified Advanced Medical Endermologie® Therapist.
A gentle way to support healing
If you are living with discomfort, restriction or visible irregularity around a scar, you deserve options that feel supportive rather than invasive.
Book a Consultation & Discovery Session
A thoughtful, unrushed conversation about your goals and what support may feel right for your body.
Book your session →
A softer, more intuitive way to recover and reconnect.
With warmth,
Niamh x
References:
1. Watson, J., & Shaw, W. Physiological Effects of Endermologie®: A Preliminary Report. Aesthetic Surgery Journal. 2. Kołodziejczak, A., Adamiak, J., & Rotsztejn, H. Endermologie as a Complementary Therapy in Medicine and Surgery.Applied Sciences 2025. 3. Waked, I. S., & Ziethar, M. M. Endermologie vs low-level laser therapy on post-mastectomy lymphedema. MJCU.
Further reading: treating c-section scars:
This episode of Beyond the Mirror dives deep into redefining self-care and wellness for women navigating the changing stage of life of peri-menopause and menopause.
It’s a time of significant change – physically, mentally, and emotionally. Maybe your metabolism is slowing, your energy levels are lower, and what used to work just isn’t effective anymore.
You might be questioning your worth or feeling lost after years of focusing on others.
Join us as we explore how to slow down, tune into your body’s needs, and shift from being others-focused to truly self-focused.
Discover why balancing hormones, adapting movement, and finding purpose become crucial.
This isn’t about reversing time, but about supporting your body, connecting with yourself, and ageing with grace, love, and compassion. Listen to the podcast HERE.
#womenintheir40s #bodyacceptance

Y’all have heard me found on about our glymphatic system before. This is why it’s important.
Repost from @newscientist A device that massages the face and neck (e.g. ENDERMOLOGIE) boosts the brain’s waste disposal system, suggesting it could reduce the severity of conditions like Alzheimer’s disease.
Cerebrospinal fluid (CSF) bathes our brain, pumped into it before leaving through a network of thin tubes called glymphatic vessels. Studies in mice have shown that this fluid flushes out waste products made by brain cells, including beta-amyloid, a protein linked to conditions such as Alzheimer’s and Parkinson’s disease.
Image: Phanie/Sipa Press/Alamy
Thanks again to Julie @eternalwellbeingcanberra for creating her magic and bringing our “chats” to air! In this week’s episode we discuss a topic that both of us discuss with our Clients regularly – belly fat!
Why does belly fat become such a struggle as we age? In this episode of Beyond the Mirror, we explore the real reasons behind stubborn belly fat in midlife, including hormonal shifts, stress, sleep, emotional patterns, and postpartum changes.
We break down why conventional advice often fails women during perimenopause and menopause, and offer a more holistic, compassionate path forward. From breathwork and strength training to nutrition, mindset, and Endermologie, this episode is a powerful reminder that your body isn’t broken. It just needs a different kind of support.
It’s time to work with your body, not against it!
Listen to the full episode HERE
I know I haven’t mentioned lymphodema (‘lymphedema’ if you’re American) on here in a while, but it’s a topic of conversation that happens quite often in clinic.
There are different types of lymphoedema and for many people conservative management (e.g. compression, lymphatic drainage – either manually or using Endermologie, compressive pumps etc.) is the mainstay of treatment. But, some people may be candidates for surgery.
This is a long-winded way to say, if you, or anyone you know has lymphoedema, this article explains how this lymphovenous bypass (LVB) or vascularised lymph node transfer (VLNT) surgery can restore lymphatic flow and drainage in some people with lymphedema.
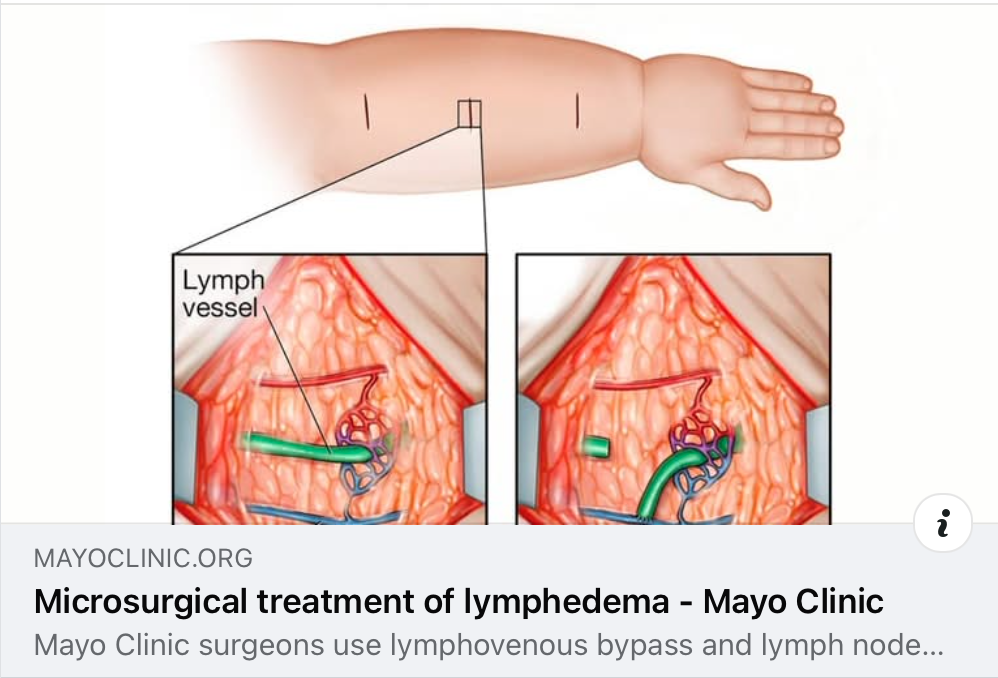
You can read the article by clicking on the link here:
If you don’t have time, here’s a quick summary:
- Context: Lymphedema is a chronic condition typically managed by conservative therapies like compression, manual lymphatic drainage, and skin care. These help reduce swelling and infection risk but require ongoing daily effort.
- Surgical options: When conservative approaches aren’t sufficient, surgical interventions – either liposuction (for debulking) or microsurgical reconstruction – can provide more durable relief.
- Microsurgery techniques:
- Lymphovenous bypass (LVB): Surgeons connect tiny lymphatic vessels to nearby veins using supermicrosurgical tools and magnification up to 40×. It’s minimally invasive, usually outpatient, with expected limb volume reduction of ~20–30% within one year post‑surgery.
- Vascularized lymph node transfer (VLNT): Healthy lymph nodes (and their blood vessels) are transplanted from donor sites—such as abdomen, groin, back, or chin—to the affected limb. This is more invasive and often used when bypass isn’t feasible. Studies show improved outcomes months after surgery, including reduced cellulitis by a factor of 10, pain relief in 75% of patients, and 42% discontinuation of compression garments.
- Considerations: Ideal candidates are those who haven’t responded adequately to conservative care. Obesity, untreated venous insufficiency or deep‑vein thrombosis, and previous treatment noncompliance may limit eligibility.
- Research and outcomes tracking: Mayo Clinic continues to study timing, number of bypasses, surgical modes, and their impact on outcomes. The goal is to optimise patient selection and efficacy of these advanced treatments.
Bottom line
Microsurgical treatments like LVB and VLNT offer a regenerative, long‑lasting alternative when traditional lymphedema therapies fall short. LVB is minimally invasive and often effective in early stages, while VLNT may deliver substantial benefit even when bypass is not viable. Ongoing research at Mayo Clinic aims to refine which patients benefit most and improve long‑term outcomes.

Nutritional strategies for lipoedema: what the evidence says about low-carb and ketogenic approaches
What is lipoedema and how is it different to obesity?
Lipoedema is a chronic, painful condition that causes disproportionate, symmetrically distributed subcutaneous adipose tissue — usually in the legs, buttocks and sometimes arms. It almost exclusively affects women, with approximately 11% to 39% of adult women affected. The large range is explained by poor access to diagnosis because lipoedema is often confused with obesity or lymphoedema (or occasionally Dercum’s disease or lipomatosis). However, there are some key clinical and metabolic differences between these disorders.1
Lipoedema causes pain, bruising, swelling and reduced mobility. Hormonal alterations and genetic components, such as the AKR1C1 gene mutation, are thought to play a role in its pathophysiology (i.e. the functional and biochemical changes that are associated with/or a result of disease).2
The adipose tissue accumulation in lipoedema is resistant to lifestyle interventions. In one study, patients with lipoedema were found to have larger adipocytes (fat cells) as well as enlarged/dilated blood and lymph vessels, contributing to issues like swelling and poor circulation.3 It’s also been found that angiogenesis (formation of new blood vessels) occurs in lipoedema, suggesting that the body is trying to supply more blood to the area, possibly due to increased metabolic demands or tissue stress. Lipoedema tissues have also been shown to contain more macrophages (immune cells that help fight infections and clear away dead cells), indicating ongoing inflammation or tissue repair.3
This supports the view that lipoedema is not just a cosmetic issue actually involves complex changes in the tissue; including blood and lymph vessel abnormalities, increased immune activity, and altered fat cell structure.4,5 Also, chronic inflammation observed in lipoedema may lead to fibrosis – an excessive connective tissue buildup that causes tissue stiffness and reduced flexibility. Some clinicians describe lipoedema as an “adipofascial” condition6,7 or “fibrotic loose connective (adipose) tissue (LCT)” disorder.5
‘Treating’ lipoedema with diet
While there is no cure for lipoedema, emerging research suggests dietary approaches aimed at lowering insulin and systemic inflammation can improve symptoms. A 2024 consensus guideline by German vascular, lymphology and phlebology societies supports using low-carbohydrate and ketogenic diets as part of a multidisciplinary strategy.8
These nutritional approaches are biologically plausible because insulin signalling, steroid hormones, and adipose metabolism play roles in lipoedema’s pathophysiology. This article also examines alternative dietary strategies and explains how LPG Endermologie can work as a complementary therapy to support people with lipoedema.
What the ketogenic / low-carb evidence shows
Several recent clinical studies and reviews report symptomatic improvements in people with lipoedema who follow low-carbohydrate or ketogenic diets, including reductions in pain, limb circumference, and subcutaneous adipose tissue, along with improved quality of life.9,10
- The LIPODIET pilot study (University of Oslo) found that a ketogenic approach was associated with reduced pain and better quality of life in patients with lipoedema, even when weight loss did not fully explain symptom changes. However, this study involved only nine women and ran for seven weeks, so the authors noted that larger randomised trials are required to confirm these findings.10
- A 2020 prospective study found that a carbohydrate-restricted, anti-inflammatory diet led to measurable improvements in limb pain, swelling, and tissue tightness, suggesting metabolic regulation may benefit microvascular and lymphatic function. 11
- A randomised, 8-week low-carbohydrate vs. low-fat trial reported that the low-carb group (75 g/day) had significant reductions in calf subcutaneous adipose tissue area, calf circumference, and pain compared with the higher-carb (185 g/day) control, despite identical calorie intake (1,200k/cal daily).12 This was one of the first randomised dietary trials in people with lipoedema, but again numbers were low – only 13 in total of which 5 were in the low-carb group.12
- A 2023 review of very low-calorie ketogenic diets (VLCKD) identified potential for reducing inflammation which is a key contributor to lipoedema’s pathogenesis.13
- Narrative and systematic reviews* emerging in 2024 – 2025 summarise multiple small studies, reporting that ketogenic and therapeutic carbohydrate-restricted diets show promise for reducing inflammation, pain, and local adiposity, though larger, longer trials are needed.14–16
What clinicians and guidelines say
The 2024 German S2k guideline emphasises that lipoedema is a complex adipose-tissue disorder and recommends an individualised, multimodal management approach including conservative measures, compression, physiotherapy, dietary modification, and surgery where appropriate.8 They emphasise that diet is one component of symptom management but not a cure. Guidelines and expert groups stress individualised care and multidisciplinary (medical team) oversight. 8
Why keto / low-carb might help
Low-carbohydrate or ketogenic diets may benefit lipoedema through several overlapping mechanisms. By reducing insulin signalling, they may help limit further abnormal fat accumulation. Nutritional ketosis also has systemic anti-inflammatory effects, which may reduce fluid retention and improve microvascular and lymphatic function.17
Many patients report less pain, reduced heaviness, and improved mental clarity and sleep within days to weeks, though responses vary. Several small studies have outlined these mechanisms and observed measurable improvements, supporting the role of diet as a complementary therapy in lipoedema care.17,18
Risks, unknowns and reasons for careful supervision
No diet is risk-free. Some research, particularly in athletic populations, has raised concerns about about short-term effects of strict ketogenic diets on bone health and other markers.19 Unfortunately, long-term safety data for strict ketogenic diets in people with lipoedema are limited. Some people with medical conditions or taking medications should only start a ketogenic plan under medical supervision and ideally with a registered dietitian with experience in lipoedema and low-carb therapeutics.
Alternatives & hybrid approaches
Not every person with lipoedema benefits from strict ketogenic eating. Reported alternatives that benefit some people with lipoedema include:
- Low-carbohydrate (not strict keto). 50 – 100 g/day may be more sustainable and still effective.12
- Mediterranean diet. In one study, patients’ weight was significantly decreased, including in the affected limbs, after 4 weeks and they reported improved quality of life with less fatigue, pain and anxiety.20
- Intermittent fasting (time-restricted eating). Evidence suggests fasting 18 hours with a 6-hour eating window cantrigger a metabolic switch from glucose-based to ketone-based energy, with improved stress resistance, increased longevity, and a decreased incidence of diseases, including obesity.21,22 However, some nutritionists warn against restricted eating for people with lipoedema.23
- Rare Adipose Disorder (RAD) diet. Elimination of high-glycaemic-index (GI) foods and sugars – including gluten and processed/refined carbs. The emphasis is on organic whole foods and healthy fats. Long term compliance could be difficult and lead to yo-yo dieting – potentially doing more harm than good.24,25
- Elimination or low-FODMAP diet. Restricting foods high in fermentable carbohydrates (FODMAPs = Fermentable Oligosaccharides, Disaccharides, Monosaccharides, And Polyols, which are poorly absorbed sugars) and replacing them with low-FODMAP alternatives for 2–6 weeks. Then systematically reintroducing different FODMAP groups, testing for reactions to find personal food triggers.26
Note: clinical trials directly comparing multiple diet styles are few. The best approach is individualised: choose a diet that can be relatively easily sustained, improves symptoms, and is medically safe.
How Endermologie complements dietary approaches
Endermologie (medical mechanised massage/myofascial and lymphatic stimulation using LPG devices such as the Cellu M6 Alliance) is commonly used as an adjunct therapy for symptom relief in lipoedema. Evidence indicates it can:27–29
- Improve lymphatic flow and reduce fluid-related swelling and heaviness
- Reduce local fibrosis and improve soft-tissue mobility
- Improve skin quality and appearance of cellulite/resistant fat
- Provide symptomatic relief and improved function when combined with conservative care such as compression and exercise.
Comparative studies found Endermologie and manual lymphatic drainage (MLD) both beneficial for lymphatic conditions withmeasurable reduction in circumference and skin quality improvements after short treatment courses. 30,31 Combining a nutritional strategy with Endermologie, compression, and exercise forms a multimodal, evidence-based strategy.
Practical guidance
- Talk to your clinician first. Always seek medical advice before starting a low-carb or ketogenic plan – especially ifyou have diabetes, kidney disease, or take regular medications.
- Prioritise whole foods. Reduce sugars and refined carbohydrates, avoid processed foods such as white bread, confectionery, fast food and sugary drinks etc. Instead aim for nutritious meals including healthy fats like avocado, nuts, fish and olive oil.
- Combine with conservative care. Use compression garments and/or pneumatic pumps, exercise, and lymphatic-focused therapies such as Endermologie.
If you’re managing lipoedema and curious about dietary approaches, speak with your GP or a qualified dietitian. If you’re already working with Endermologie or considering it, combining a tailored nutrition plan with regular Endermologie sessions, compression and gentle exercise is a practical, evidence-informed pathway many patients find helpful
* Narrative reviews are expert summaries (e.g., in Medical Hypotheses, Nutrients, or Obesity Reviews) that discuss mechanisms, patient experiences, and early clinical data. Systematic reviews (e.g., in MDPI Nutrients or Lymphology journals) methodically searched databases and summarised all available studies on diet in lipoedema.
References
- Forner-Cordero, I., Szolnoky, G., Forner-Cordero, A., & Kemeny, L. (2012). Lipedema: An overview of its clinical manifestations, diagnosis, and treatment of the disproportional fatty deposition syndrome – systematic review. Clinical Obesity, 2(3–4), 86–95.
- Michelini, S., et al. (2020). Lipoedema: Genetic and molecular mechanisms. International Journal of Molecular Sciences, 21(24), 9026.
- Al-Ghadban, S., Cromer, W., Allen, M., Ussery, C., Badowski, M., Harris, D., & Herbst, K. L. (2019). Dilated blood and lymphatic microvessels, angiogenesis, increased macrophages, and adipocyte hypertrophy in lipedema thigh skin and fat tissue. Journal of Obesity, 2019, 8747461.
- Kruppa, P., et al. (2022). Adipose tissue characteristics of lipedema: The disease of the adipose tissue. Plastic and Reconstructive Surgery Global Open, 10(12), e4754.
- Suga, H., et al. (2021). Fibrotic loose connective tissue in lipedema. Cells, 10(12), 3468.
- Poojari, V., et al. (2022). Adipofascial changes in lipedema: A histological analysis. Obesity Surgery, 32(10), 4050–4062.
- Suga, H., et al. (2021). Cells, 10(12), 3468. [reaffirmed for “adipofascial” context]
- German Society of Phlebology et al. (2024). S2k guideline: Lipedema – Diagnosis and treatment (AWMF 037–012l).
- Wolf, S., et al. (2024). Low-carbohydrate and ketogenic diet interventions in lipedema: A review. Obesity Reviews, 26(3), e1258.
- Hofsø, D., et al. (2021). Ketogenic diet improves pain and quality of life in lipedema: The LIPODIET pilot study. Obesity Science & Practice, 7(6), 623–631.
- Karasu, S. R., et al. (2020). Clinical effects of a carbohydrate-restricted diet in women with lipedema. Nutrients, 12(12), 3865.
- Frontiers in Nutrition. (2024). Randomised trial comparing low-carbohydrate vs low-fat diets in lipedema. Frontiers in Nutrition, 11, 1484612.
- Muscogiuri, G., et al. (2023). Very low-calorie ketogenic diet and inflammation modulation. Current Obesity Reports, 12, 42–56.
- Pohl, R., et al. (2024). Ketogenic diet and lipedema: Systematic review. Nutrients, 16(19), 3276.
- ScienceDirect (2025). Therapeutic carbohydrate restriction in chronic adipose disorders: Review of emerging evidence. Nutrition Research Reviews, 38(1).
- Springer (2025). Narrative review: Ketogenic interventions and inflammation in adipose disorders. Obesity Reviews, 36(2).
- Paoli, A., et al. (2021). Ketogenic diet mechanisms in chronic inflammation. Life, 11(12), 1402.
- Tóth, C., et al. (2020). Pain and inflammation reduction in lipedema with nutritional ketosis. Medical Hypotheses, 144, 110037.
- EatingWell Editors. (2024). The keto diet could be bad for bone health, study says. EatingWell Magazine.
- Vetrano, D. L., et al. (2021). Mediterranean diet and adipose tissue reduction in chronic disorders. Nutrients, 13(2), 291.
- Sutton, E. F., et al. (2018). Early time-restricted feeding improves insulin sensitivity. New England Journal of Medicine, 381, 999–1012.
- Longo, V. D., & Panda, S. (2016). Fasting, circadian rhythms, and time-restricted feeding. Cell Metabolism, 23(6), 1048–1059.
- I Choose Health. (2023). When fasting isn’t OK for people with lipedema. I Choose Health Blog.
- Herbst, K. L. (2023). The RAD Diet for Lipedema. Amazon Publishing.
- Thomas, D. M., et al. (2024). Weight cycling and adipose inflammation. International Journal of Obesity, 48(7), 1542–1553.
- Monash University. (2025). The low-FODMAP diet. Monash FODMAP Program.
- Sola, J., et al. (2024). Mechanised mechanical stimulation and lymphatic flow. Applied Sciences, 15(8), 4313.
- Querleux, B., et al. (1999). LPG Endermologie and lymphatic circulation. Journal of Cosmetic and Laser Therapy, 1(2), 83–90.
- Wanitphakdeedecha, R., et al. (2020). LPG endermologie for improving cellulite and skin quality: A review. Dermatologic Therapy, 33(6), e13973.
- Leduc, O., et al. (2015). Comparison of manual lymph drainage and LPG techniques in lymphoedema. Revue de Lymphologie, 67, 23–29.
- Wounds International. (2024). Multidisciplinary management of lipedema. Wounds International Journal, 15(3), 44–50

